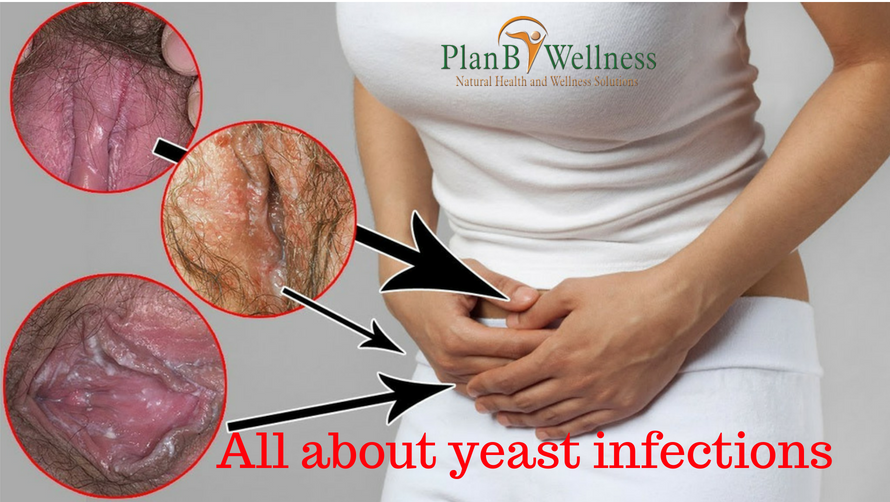
Most women — and some men — will have a yeast infections at some point in their lives. Also called candida vaginitis or vulvovaginal candidiasis. Yeast infections are most commonly caused by the fungus candida albicans.
They can also be caused by other Candida species, including C. glabrata, C. parapsilosis, C. tropicalis, andC. krusei.
Up to 75% of women will get a vaginal yeast infection at least once in their lives and 40 to 50% of women will experience more than one infection, according to a 2007 article in the medical journal ’The Lancet’’.
What’s more, 5 to 8% of women experience recurrent or chronic yeast infections and come down with four or more yeast infections in a single year.
Additionally, men can get yeast infections in their genitals, mouths and other areas too.
Though the term “yeast infection” is most often used to refer to a vaginal infection, it also applies to other types of candidiasis. A yeast infection of the mouth is called thrush, or oropharyngeal candidiasis. A yeast infection of the skin — which typically occurs in warm, moist areas, such as the armpits and groin — is called cutaneous candidiasis. If Candida gets into the bloodstream, such as from using a contaminated intravenous catheter, the yeast can cause a deadly infection called invasive candidiasis.
Causes of Yeast Infections
Candida yeast causes an infection when something throws off the balance between the microorganisms that live in and on your body, such as:
- Pregnancy
- Certain medications, including birth control pills, antibiotics, and steroids
- Immune-suppressing diseases, including HIV
- Diabetes
- Obesity
- Stress and lack of sleep, which can weaken the immune system
Additionally, certain lifestyle habits may also promote the growth of Candida, including:
- Eating a diet high in sugar (a yeast food source)
- Using scented soaps, bubble baths, and feminine sprays
- Douching, IUD use
- Maintaining poor vaginal hygiene
- Wearing clothing that keeps the vaginal area warm and moist, such as synthetic underwear, pajama bottoms, and tight jeans or spandex
Yeast Infection Complications
Some types of candidiasis or yeast infections can lead to serious health problems if left untreated. Also, yeast infections are a frequent complication of other conditions, such as female infertility.
Thrush: Oral candidiasis, or thrush, is rarely an issue for healthy children and adults.
If you have a compromised immune system, such as from HIV or from persistent steroid use, thrush can lead to life-threatening systemic infections. Over time, the yeast may enter your bloodstream — a condition called invasive candidiasis — and travel to other parts of your body, including your lungs, liver, and heart valves.
Invasive candidiasis, which is also sometimes caused by contaminated catheters, can ultimately cause organ failure and death.
Pregnancy: Vulvovaginal candidiasis is especially common among pregnant women. Because of this, the infections are sometimes considered a complications of pregnancy.
Pregnancy increases your risk of getting yeast infections because of hormonal changes — high oestrogen levels likely help Candida grow. Additionally, vaginal secretions during pregnancy have higher concentrations of sugar, a food source for yeast.
The symptoms and severity of yeast infections are no different during pregnancy; they are also treated the same way in most cases.
Diabetes: Vaginal yeast infections are also considered a complication of type 2 diabetes, as the metabolic disease makes you more susceptible to the infection.
Diabetes mellitus also makes you more prone to infections by the azole-resistant species of yeast, C. glabrata. If your diabetes is uncontrolled, you’ll have high levels of sugar in your blood, which also affects the levels of sugar in other areas of your body.
Specifically, the mucous membrane in the vagina and vulva become saturated with sugar, allowing Candida to rapidly reproduce.
The risk of vulvovaginal candidiasis is not greater for women who have well-controlled diabetes, though a diet high in refined sugars may contribute to a diabetic woman’s risk of yeast infection, according to a 2007 article in ‘’The Lancet’’.
Women with diabetes and vaginal yeast infections may require longer courses of treatment than women without diabetes.
What are your greatest challenges concerning yeast infections? Tell us using the comment box below?
If you have gained anything from reading this, don’t hesitate to share it with others too. Put your comments and questions or topics you will like us to write about in the comment box below.
Stay Healthy And Never Give Up!
Plan B Wellness
Whatsapp: +2348099666658, +2348099666648
Call/text: +2348099666650
Instagram: @planbwellness
Email – consult@planbwellness.com





[…] yeast infections […]
Please how can i get your WhatsApp number or your location
Here are our wahstapp lines; 08099666648, 08099666658.
Thanks
Yes
Nice
What causes cheese like discharge days before period? Is it normal
That’s not normal madam, especialy if you are experiencing itching and burning sensations alongside the discharge. You may want to run a test to rule out yeast infection or any other infection.
If you need a natural way to overcome yeast infection or any other type of infection, click here.
I think i have some of these infection can I get halp here
Yes madam, you can.
To get our remedy that works for all forms of infections, kindly chat with our support team on whatsapp on +2348099666648 or +2348099666658
Thanks
Plan B Wellness